BACKGROUND
Founded in 1949, the Canadian Association of Pathologists – Association canadienne des pathologistes (CAP-ACP) is a voluntary professional organization that aims to advance the interests of the profession and promote high-quality standards for patient care by providing national leadership and promoting excellence in pathology and laboratory medicine practice, education, and research.1 Since its inception, the organization has expanded to boast eleven special interest groups, nine standing committees, four sections and seven subsections.
The unprecedented nature of the COVID-19 pandemic overwhelmed many parts of the healthcare system. In particular, COVID-19-related examinations had increased to a point where the workload overloaded pathologists.1–5 To maximize efforts in combatting the pandemic, many hospitals and laboratories diverted resources away from routine surgeries and laboratory testing. Routinely tested cases were no longer reviewed as the government put them on hold. Due to these demands, a cohort of residents had a significant reduction in case exposure, with some reporting detrimental impacts on their training and diagnostic abilities.6,7 The CAP-ACP Virtual Education Series emerged from a need to offer education during the pandemic, when the demands on pathologists made it impossible to leave the lab and travelling for in-person conferences was halted. Giving small one-hour doses of virtual education became a way for pathologists to listen and work simultaneously and provided a consistent platform to expose residents to cases that they would see again after the pandemic.
To date, CAP-ACP has hosted 115 virtual education webinars accredited as Section 1 activities by the Royal College of Physicians and Surgeons of Canada. Using a mixed methods analysis of the results of post-activity surveys of these webinars, this paper aimed to examine pathologists’ perceptions of the webinars and explore significant themes in qualitative responses.
METHODS
Study design
Using a convergent mixed-methods design, data from 115 post-session continuing medical education (CME) evaluation surveys were analyzed. The quantitative and qualitative results were analyzed separately. Integration occurred during initial data collection, interpretation, reporting, and discussion levels using a weaving approach.8 The study methods were entered into the ARECCI Ethics Screening tool and earned a score of 0. Therefore, Research Ethics Board approval was not required.
Study participants
Participants included CAP-ACP webinar attendees. While the surveys did not collect identifying or demographic information beyond geographic location from attendees, the qualitative responses suggest that pathologists and pathologists’ assistants were the primary demographic. During the pandemic, CAP-ACP membership increased, as did attendance of the webinars.
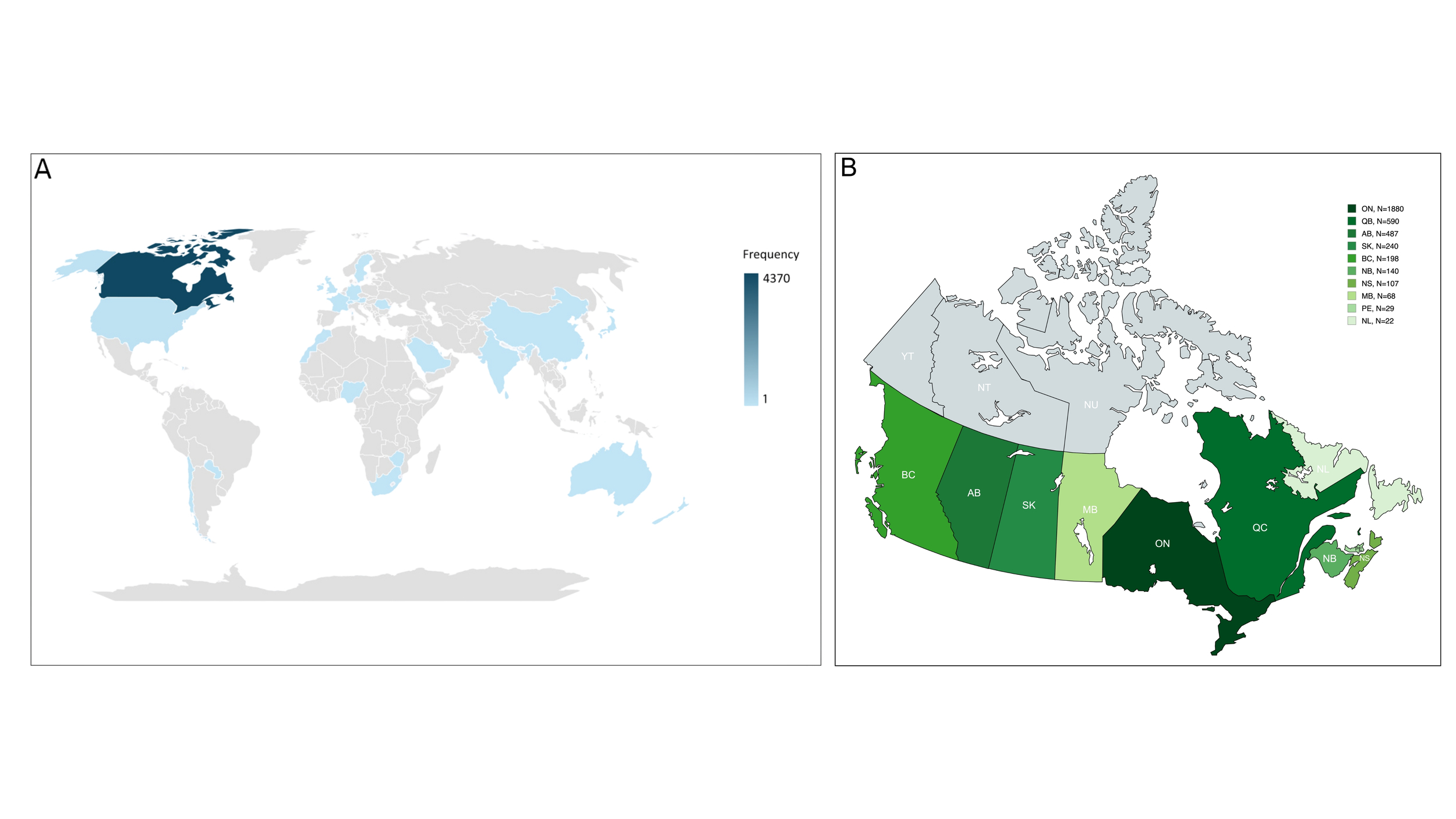
The online webinars reached participants across the globe, including from Africa, Asia, Saudi Arabia, and Europe (see Figure 1A). Canadians comprised 93% of participants, with representation from other countries: 1.7% from the United States, 1.2% from Qatar, and 1.5% from Taiwan.
Among Canadian participants, 96% provided their city information, resulting in a list of 172 different Canadian cities. The most frequently reported cities were Toronto (11.8%), followed by Edmonton (6.7%), Montreal (6.1%), Saskatoon (4.7%), Calgary (4.5%), and Hamilton (4.3%) (see Figure 1B).
Survey tool and data collection
An anonymous online survey tool was used to assess the quality of the CME activities as per CAP-ACP’s requirements for Royal College Section 1 activities. Questions included both quantitative and qualitative responses assessing participant perceptions of the CME activity, such as whether it met the learning objectives, how it would impact competency and practice, and suggestions for the future.
Data analysis
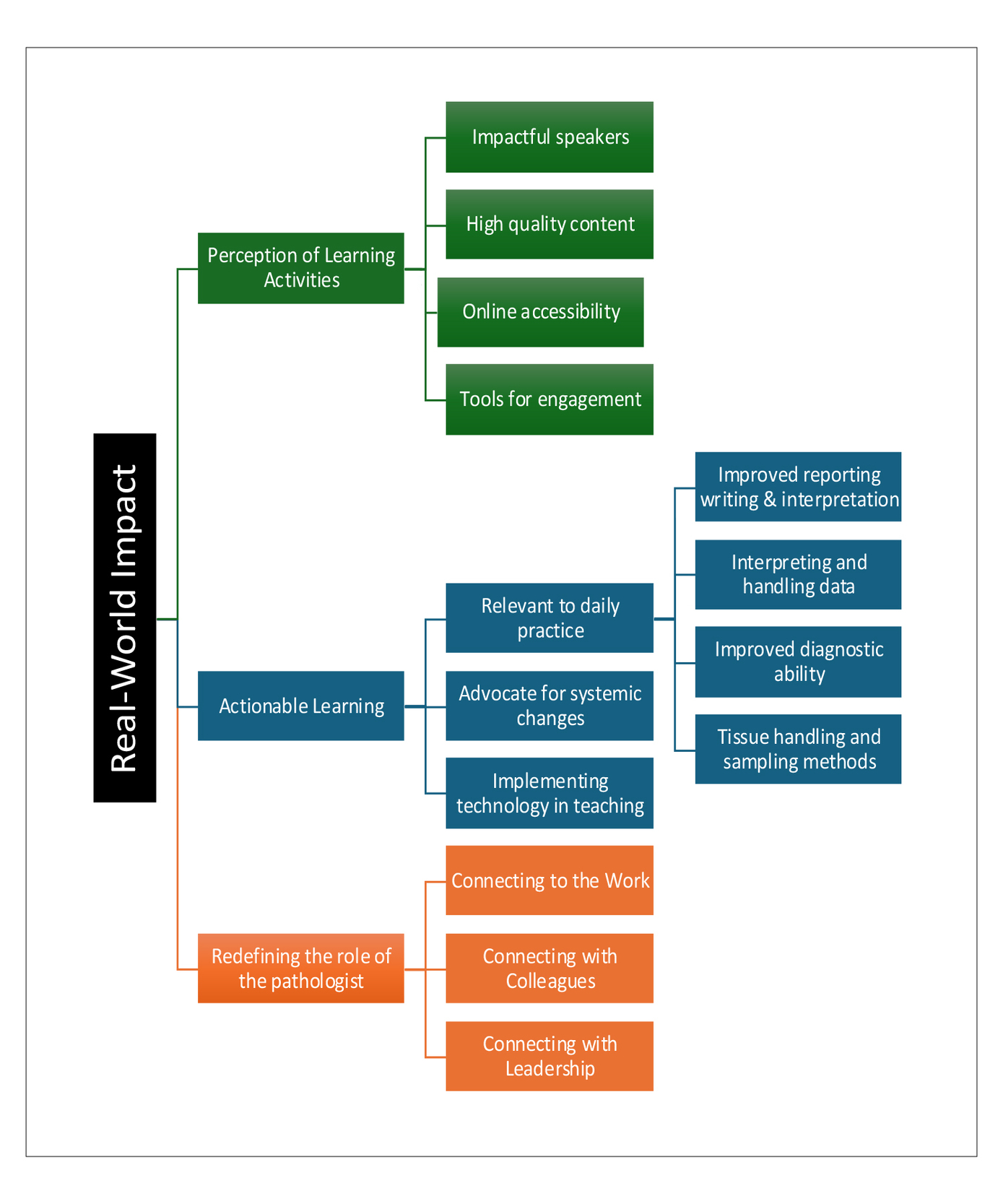
Quantitative data analysis was conducted using descriptive statistics in Microsoft Excel. Qualitative data was analyzed using an inductive thematic analysis was completed using a codebook approach. All narrative comments were independently coded by two authors (BS, HD). Codes were discussed as a group with the coding authors. The manuscript was given to two pathologists for feedback for member checking and edited in light of their responses. The codebook was subsequently revisited and re-evaluated, considering these discussions, to produce a final thematic map (Figure 2).
RESULTS
Three primary themes were developed throughout the analysis:
-
Participant perception of learning activities (subthemes: accessible, engaging, impactful);
-
Small doses of actionable learning (subthemes: relevant to daily practice, supporting systemic changes, equipping lecturers in a digital world); and
-
Pathology at a crossroads (subthemes: connecting to the work, connecting with colleagues, connecting with leadership).
Italicized quotes in this section were taken from post-activity feedback of participants.
1. Perception of learning activities
Accessible
Despite its beginnings as a safety measure during the COVID-19 pandemic, the accessibility of virtual education continues to minimize geographical and financial barriers.
Just to say thank you for an excellent series of educational seminars. This format is so much more accessible to the membership for whom travel is a burden and I really hope it continues even after it is safe to have large meetings. Different types of learning activities make this a very inclusive organization. Kudos again.
In an era of rapid advances and a field in which time constraints hinder keeping current with new information, pathologists valued the convenience and quick access to learning.
The world of oncology is progressing at a breakneck speed and (we) pathologists have to keep up with this advancement to have meaningful conversations with our oncology colleagues. This is especially important to those of us in community/ general practice. These days it is very challenging to keep up to date with all information. So, webinars such as this one [are] very helpful in giving background and distilling essences of the various taskforce recommendations.
Engaging
Lecturing online included new developments in enhancing engagement in webinars. Participants, “love the interactive format of the breakout rooms, working through cases as a team.” Another participant enjoyed the “voting for answers. Kept us involved” through the polling feature.
Question and answer components are a highly valued aspect of webinars. Some enjoyed technical discussions, “the thorough discussion of common lesions and their clinical significance,” while others felt encouraged to engage in difficult conversations:
This talk was extremely insightful and provided a framework in which to process the multitude of moral dilemmas encountered on a regular basis. I appreciated the encouragement to speak openly with others rather than keep silent in shame/guilt. Great topic, thanks!
Conversely, some webinar participants called for extended question time. One remarked, “A great CME event but the question time was a bit limited.” Another shared their feedback, saying, “Great session. More time allocated for questions would be my only comment.” Participants value moving away from didactic learning to embracing an interactive, discussion-based approach.
Impactful
Participant responses consistently reflected being inspired, excited, and engaged by the lecturers. One participant expressed, “This was one of the best educational sessions I have ever attended.” A second agreed:
Excellent speaker. Very clear. Points well emphasized and well-illustrated. Allowed time for the information to soak into my head. Simplified complex area.
Despite their short, bite-sized length, the doses were potent, “I learned more about dermpath in the last 1.5 hours than in my entire career.”
Working in an often solitary profession, participating pathologists felt connected to a broader community of peers through the webinars.
Big thank you for your leadership and collegiality at all levels. As always comprehensive, practical and useful presentation - as if you can read our minds.
Participants expressed an appreciation for feeling connected to the lecturer and a desire for the spirit of belonging among peers. Competent lecturers were able to establish rapport and effectively engage with participants online.
Very effective - loved his style and connection to the audience
Webinars remove many attendance barriers and can rapidly disseminate information without detrimental impacts on learning. The overarching consensus from participants was that these sessions should be hosted regularly.
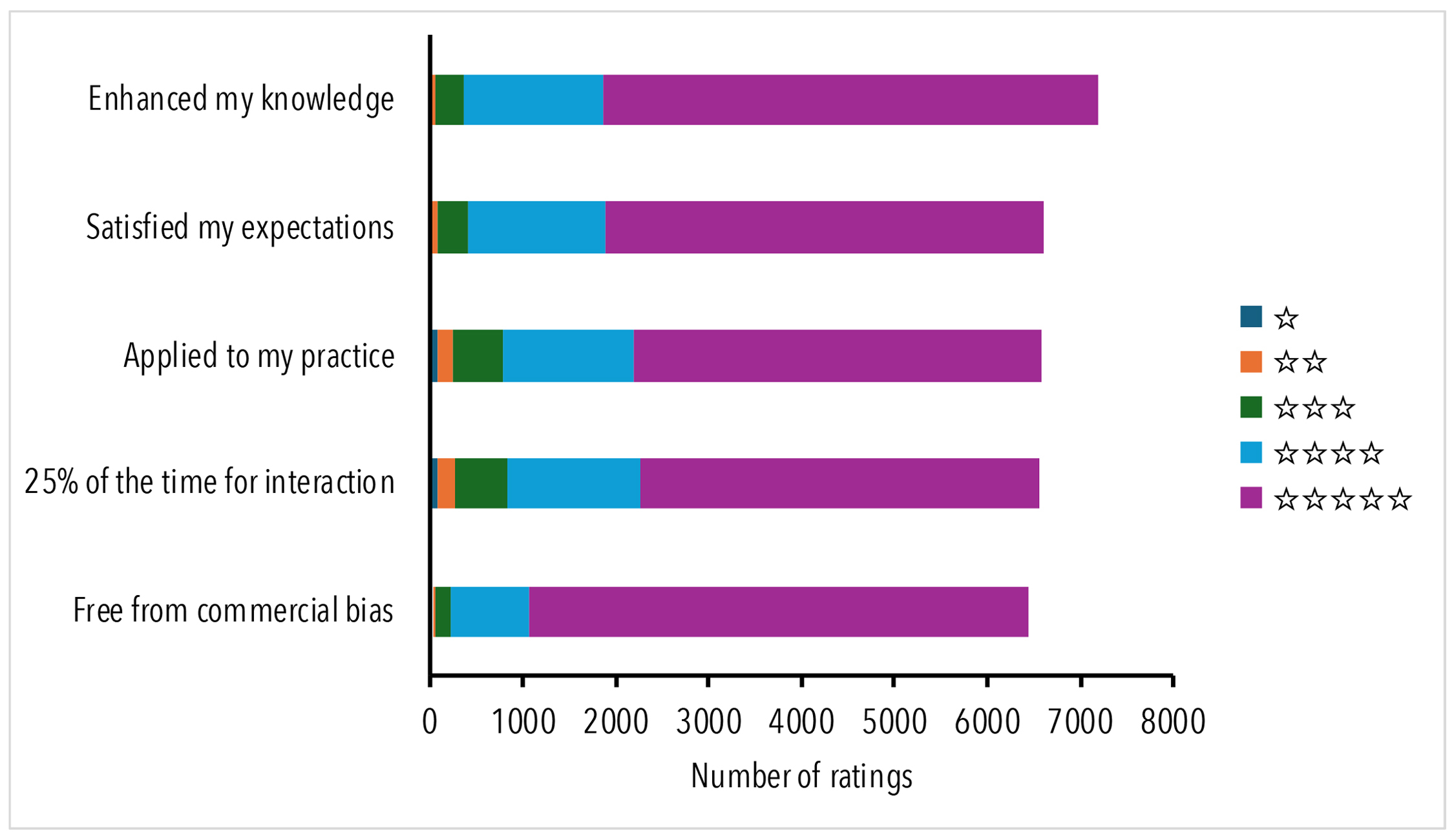
Satisfaction with learning activities was reflected in quantitative ratings of the learning activities which were rated on a five-star scale (see Figure 3). The results showed median and modal scores of 5 across all categories, indicating that webinars met stated learning objectives and fulfilled participant expectations.
2. Small doses of actionable learning
Relevant to daily practice
The theme “small doses of actionable learning” underscores the importance of practical, implementable knowledge directly tied to daily practice—a quality participants consistently valued in the webinars.
We appreciate having more webinars like this, which are closely aligned with our day-to-day work.
Key outcomes included "improved reporting," and better accuracy, clarity, and consistency in communicating prognosis and uncertainty to physicians.
My report may be more complete now that I know some more tools to guide my reporting.
These small doses of learning boosted confidence in challenging areas such as handling molecular data. Webinar insights enhanced understanding of “variance nomenclature” and the ability to “interpret molecular reports more quickly.” One participant highlighted the value of reviewing specific conditions:
I learned how to approach […] inflammatory skin lesions, how to differentiate them depends on what features I see, how to report - I learned everything that I need to know to improve my diagnostic skills.
Many participants responded that they valued lectures that taught about the nuances and pitfalls when diagnosing certain conditions:
The update on the association of HPV with neuroendocrine carcinomas of the head and neck. I found this interesting as a pitfall that I have seen during my training and my practice is that p16-positive immunophenotype does not always confirm that a malignancy is a squamous cell carcinoma.
The topic-specific focus of the webinars highlighted practical and nuanced learning opportunities that often extend beyond the scope of a traditional university education.
Supporting systemic changes
Practical applications of webinar learning extended beyond the lab to enhancing participants’ skills in leadership and decision-making:
Helps me be more effective as a medical leader by providing ideas for improving lab service through data analysis and utilization.
Following webinars, participants indicated their intention to re-evaluate current, system-wide approaches, refine their techniques, or explore alternative ways of accomplishing laboratory objectives. One participant highlighted how the learning experience inspired them to reconsider institutional practices, potentially leading to more comprehensive diagnostics:
Entities to be aware of in gynecological frozen sections that I may not have considered. In our institution, we only take 1 section on ovarian tumors, and I think this session will open a discussion on whether we should be taking 3 sections upfront on all ovarian masses.
These system-wide changes could profoundly impact patient outcomes. For example:
Improving biospecimen quality and tumour sampling for molecular analysis will maximize testing efficacy which will benefit subsequent patient management.
By leveraging data insights, participants aimed to enhance diagnostics and advocate for personalized care:
Conducting a more thorough investigation into the patient’s prior medical history before I do the gross dissection.
This data highlights that the role of pathologists is expanding in driving systemic improvements for better patient outcomes.
Equipping lecturers in a digital world
Participants highlighted the value of learning to leverage technology and online platforms to enhance their teaching practices. Lecturers valued webinars covering:
The challenges of virtual learning and how to overcome them. Also to take advantage of these new platforms to enhance learner’s experience compared to in person learning.
Another participant emphasized the importance of online as a lecturer operating in a digital world:
Online and technical info which is very important especially during these times. Glad that we have experts helping to move the profession forward when things have to be from a distance.
I’m thinking that we should maybe switch to Zoom, from MS Teams, the annotate feature is quite interesting. Also the polling feature. I like to make my sessions interactive, partly so I don’t have to talk as much and it’s been really hard for me to adjust to online because of that. I can’t see faces or gestures so I can’t build on what people are doing.
The webinars foster a desire for continuous improvement. By embracing these opportunities, lecturers are better equipped to navigate evolving conditions and inspire innovation within their institutions.
3. Pathology at a crossroads
Connecting to the work
Responses revealed a strong desire for pathologists to reconnect with the clinical significance of their work. Quantitative responses (Table 1) showed that 80% felt the webinar enhanced competence, but only 66% believed it would impact patient outcomes, indicating a disconnect between laboratory specialists’ work and its perceived effect on patient care.
One participant noted, “[The webinar put into perspective] why I order these tests.” Another writes:
As a path assistant at a hospital that specializes in high-risk pregnancies, I gross an exorbitant amount of placentas. Because of the high volume, grossing them becomes very routine and redundant so this session was a good reminder of the clinical relevance in placental examination.
The repetitive nature of a pathologists’ assistants’ (PA’s) work can become monotonous without the context of patient care. For this PA, the webinar invoked a broader meaning – that each placenta is not routine, but critical to a mother and a child. They are part of something beyond the lab.
Connecting with colleagues
Certain participants expressed that they are increasingly viewed as technicians rather than medical doctors.
Pathologists are losing ground to other specialties. They are losing their name and role as doctors. […] Pathology practice should be patient-oriented, like sample collection and talking to the patient, as the radiologist does.
This participant expressed a need to reaffirm their role as integral members of the medical team through recognition of their contributions by colleagues and patients. While patient contact is one way of enhancing their sense of meaning, survey results support the integration of pathologists into multi-disciplinary teams. Following the webinars, participants acknowledged the need for “clear[er] language and communication in pathologic diagnosis.” One participant remarked, “I was not aware of 30% misinterpretation from pathologist to surgeon.” High misinterpretation rates suggest systemic communication issues that may stem from insufficient dialogue within multidisciplinary meetings. Including pathologists in these meetings could reduce these errors.
Demonstrating their desire for interdisciplinary collaboration, pathologists valued insights into clinicians’ diagnostic approaches:
I really appreciate the comments about learning what our oncologists are thinking and how they will incorporate PD-L1 assessment in the management of their upper GI tract cancer patients.
Including pathologists within the clinical team may, therefore, combat the growing sense of devaluation and depersonalization within the profession and improve clinical decision-making, with patients being the ultimate beneficiaries. CME webinars promoted and facilitated skills required for multi-disciplinary collaboration.
Connecting with leadership
Many participants praised wellness webinars: “I loved the presentation. Very practical. I already rearranged my working environment and thank you for affirming this change.” Others raised concerns with the feasibility of these interventions, “I’ll try to start moving more during the day, rearranging my office as demonstrated, if possible.” Certain participants highlighted the need for wellness interventions to engage both pathologists and leadership teams, “low hanging fruit – rearrange the office. Pressure leadership to make wellness a priority.” The conditions engendering burnout are a shared responsibility.
Pathologists want to implement wellness initiatives in departments:
It was really cool that she talked about the financial calculator tool to justify hiring more. Huge problem here in Qc, depts are hugely understaffed. I’m always told decisions (of any kind) come down to money. I’ve been trying to bring more wellness initiatives in my dept, especially for residents as I’m one myself, and it’s been met by a lot of push back. Having data, especially pathology-specific data will help out a lot.
Willingness from pathologists is not enough for the implementation of programs, and support is required from administrative teams. There is an overarching consensus that, “We need more talks like these. More open discussion about what is plaguing the system.”
One participant voiced frustration:
[A couple of years ago, a] colleague in our department [took his life] and it was hidden and covered up and either completely forgotten or just ignored (not sure which is worse) and I feel like a strong statement from the national body may help some of us lowly worker bees to make this of importance for our departments.
This quote expresses a sense of helplessness. The phrase, “lowly worker bees” illustrates this participant’s perception of being undervalued and crises ignored. Another participant criticized the gap between rhetoric and action from governing bodies:
Organizations talk burnout but they don’t do anything about it. […] In the eyes of the government and our lab leaders, physicians are a liability and not an asset. As such topics like burnout are considered “whining”. When organizations talk about “how important physician health is” then we expect to see meaningful action - but there is none.
Referring to physicians as “liabilities” reflects this participant’s perception that authorities consider them as dispensable. Certain pathologists are disillusioned by what they identify as systemic inaction. There is a deep-rooted sense of mistrust between many pathologists and their leadership teams, which creates barriers to their engagement in wellness initiatives and peer-based support.
DISCUSSION
Webinars: Transforming CME engagement?
Participants expressed high satisfaction with learning content, praising the impactful speakers, high quality of the content, accessible delivery, and use of online learning tools to increase engagement during lectures. Other studies similarly show high satisfaction with online CME programs.9,10 In agreement with our findings, the literature indicates that interactive discussion is a powerful learning tool.11 Use of breakout rooms and polls facilitates concurrent interaction from the entire audience and allows instructors to provide prompt feedback to participants. Classroom learning is no longer unilateral but supports audience-wide participation. In this way, Waltemeyer and Cranemore11 argue that online education may surpass traditional learning opportunities.
Consistent with the literature, participants valued learning that applied to their daily practice, including improved report writing, interpretation and handling of data, improved diagnostic ability, and tissue handling and sampling methods. Reis et al.12 report that barriers to participation in CME included a lack of time, perception of work overload, lack of digital competence, and motivational and emotional factors. Conversely, they report that practical and pragmatic characteristics of online CME facilitated participation. The convenience of short, targeted learning opportunities that mitigate travel challenges, financial constraints, and the guilt associated with prolonged absences from work facilitate increased engagement.12–14
Online teaching tools can significantly enhance instructors’ teaching abilities. Cho et al.15 found that while lecturers recognize questioning techniques as critical for engaging participants, 40.4% did not use these techniques. Additionally, lack of interaction is the most cited reason for dissatisfaction among online learners.16 Our results indicated that lecturers valued webinars that taught them how to use engagement tools in online teaching to facilitate rapid and continuous audience interaction. This approach allows for class-wide engagement beyond the traditional didactic question-and-answer format. As a result, the enhanced engagement in online learning benefits both students and instructors, making webinars profoundly effective and pragmatic for CME engagement.
A need to reconnect
A central theme that emerged from the qualitative analysis indicated that, to many, the webinars held meaning beyond the bounds of academic learning and CME requirements.
Consistent with recent studies, the qualitative data indicated that burnout among pathologists is a concerning issue. Julia Keith’s17 study reported that 58% of Canadian pathologists experience burnout, and Cohen et al.18 found a burnout rate of over 47% among American pathologists. The current analysis suggests that certain pathologists perceive burnout as a systemic issue in which they are undervalued by the system. In addition, a lack of interaction within multi-disciplinary teams reduces their profession to diagnostic tasks, and there is a sentiment of loss of meaning in their work. Supporting these findings, a recent survey, including 2,363 pathologists, pathologists’ assistants, and pathology and laboratory professionals, echoed these findings, identifying workload and loss of meaning in work as the most common causes of burnout.19 These findings require further investigation and suggest systemic reforms to address the psychological and professional challenges faced by pathologists. Phenomenological and social constructionist investigations may offer deeper insights into the lived experience of pathologists and how workplace culture and systemic issues contribute to loss of meaning, respectively.
Humans possess an intrinsic need to believe that our lives hold meaning and that our actions are meaningful; when we fail to find meaning in our work, the result is often burnout.20 According to Maslach and Jackson,21 the primary causes of burnout are emotional exhaustion, depersonalization, and discontent with achievement. The qualitative analysis indicated that the webinars reminded pathologists of the clinical significance of their work and the critical importance of their work to each patient and family. To pathologists working behind the scenes, the webinars reconnected them with the meaning of their work.
Furthermore, the literature has established that strong social relationships protect against burnout, with workplace loneliness leading to psychological detachment and emotional exhaustion.22,23 Highlighting the solitary nature of many pathologists’ workdays, Roboy et al.‘s24 study indicated that 52% of a pathologist’s work time is spent in anatomical pathology and 14% in the clinical laboratory, with the remainder typically spent in teaching, research, and administration. The importance of increasing social interactions among pathologists is supported by Keith’s study17 which showed that the more time pathologists spent alone each workday, the greater their experiences of emotional exhaustion and depersonalization. Conversely, having a common area to informally converse with colleagues improved scores on the same domains. The results showed that pathologists appreciated insights into clinicians’ diagnostic processes and sparked a desire to connect within multi-disciplinary teams.
The responses indicate a loss of meaning in work and a desire for increased social interactions and recognition of the clinical significance of pathologists’ work. CAP-ACP webinars reminded certain pathologists and laboratory specialists of their critical impact on patients. National organizations such as the CAP-ACP may be able to facilitate the destigmatization of mental health issues through open discussions and encourage increased engagement with peers and wellness initiatives. In doing so, they may rebuild trust between individual pathologists and their leadership teams.
Strengths and imitations
A notable strength of this study was the immediate collection of data following each webinar, ensuring that participant feedback and interactions were captured while the CME session was fresh in their minds. Additionally, the broad scope of participants from across the pathology fraternity ensured that the findings reflected a diverse set of perspectives.
Nevertheless, there were limitations. As the study relied solely on survey responses, the depth of the analysis was limited compared to more comprehensive qualitative approaches. Additionally, participant responses may have been biased toward the specific topics of each webinar, potentially skewing the feedback to favor subjects that were more engaging or directly applicable to their preferred practice areas. Furthermore, unless disclosed we cannot discern the qualification or role of the individual making each comment.
While the study provides valuable insights into the success of CME webinars in enhancing learning and engagement, it also opens the door for further, more nuanced investigations into the critical issue of burnout in the field of pathology.
CONCLUSION
The present study highlights the high level of satisfaction with CME webinars, particularly those that successfully broke traditional barriers to learning and facilitated widespread engagement. Participants valued the interactive and inclusive nature of webinars, which supported audience-wide learning. Moreover, the ability to access content that had immediate applicability to their clinical practice was especially appreciated. Actionable learning, which could be implemented quickly in daily tasks, significantly enhanced the overall impact of the sessions.
Using online tools, such as breakout rooms, polls, and continuous audience interaction features, boosted engagement and enhanced instructors’ teaching abilities. The rapid feedback loops and class-wide participation created a dynamic learning environment, fostering an experience beyond passive information consumption. Both learners and instructors benefited from a collaborative and interactive format.
However, burnout emerged as a significant concern. Participants expressed feelings of emotional exhaustion and depersonalization, underscoring a troubling loss of meaning in their work. This finding warrants further investigation, primarily through in-depth qualitative analyses of the lived experiences of pathologists. By focusing on fewer participants but conducting a deeper exploration, future studies may uncover the complex psychological and systemic factors contributing to burnout in the pathology field.
This manuscript was peer reviewed.
Disclaimer
BS is a paid consultant for CAP-ACP who analysed the data and summarized the results into a manuscript format. HD conducted the survey on behalf of the CAP-ACP.
The authors declare that there are no undisclosed conflicts of interest regarding the publication of this paper. All authors have provided Clockwork Communications Inc. with non-exclusive rights to publish and otherwise deal with or make use of this article, and any photographs/images contained in it, in Canada and all other countries of the world.
ISSN 2819-2842